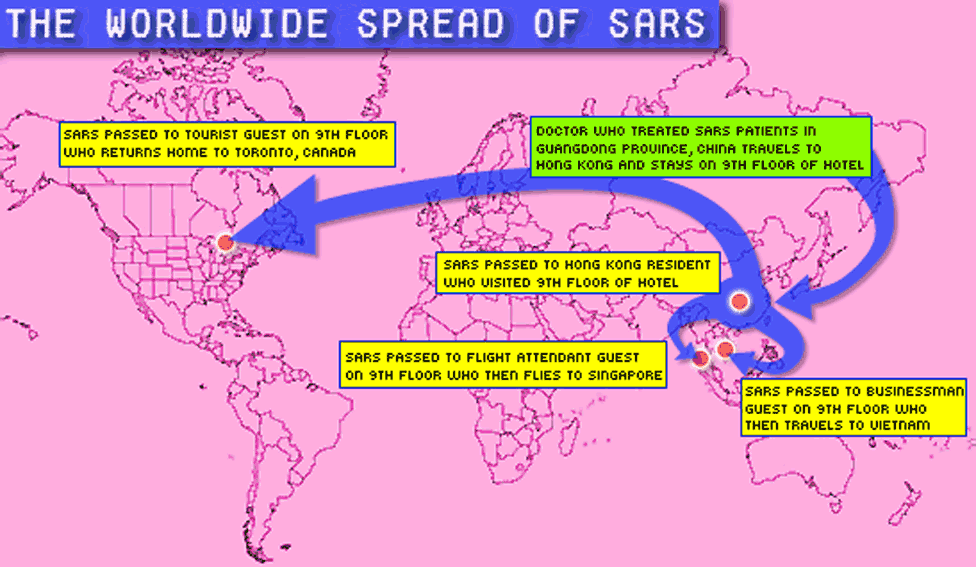
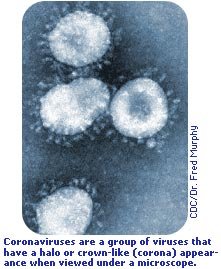
Since the turn of the millennium, new strains of deadly viruses have emerged and quickly spread around the world. We saw an outbreak of SARS coronavirus in 2003, and a much larger H1N1 "swine flu" pandemic in 2009.
Other viruses seem poised and ready to spread. Ebola Hemorrhagic Fever has sprung up in several towns in West Africa. MERS coronavirus has been found in people and camels in the Middle East. During the last decade, H5N1 "bird flu" has been killing massive numbers of wild and domestic birds each year, and in some cases it has been able to spread from birds to people.
Our changing habits seem to be helping viruses spread more quickly than they did just a few decades ago. We routinely travel by plane around the world. Someone may be exposed to a virus one day and then bring it back to their own city the next. Cities are growing bigger and denser, and we're gathering in large crowds at sport and other events.
Fortunately, today scientists can use genetic tools, such as DNA sequencing, to learn about new strains of viruses. These tools are helping researchers identify the cause of an infection, piece together a story about where new viruses come from, diagnose new cases, and develop preventive vaccines.