Types of Pain
Pain falls mainly into three categories: acute, chronic, and emotional. Each type involves distinct mechanisms and features, though they also have some in common. These categories are useful because they help us understand and talk about our experiences. But remember, pain is complex, and you’ll find examples that fall between categories.
Acute pain is sharp and sudden. It comes from a specific and immediate cause, and it is protective. We all experience acute pain. Bumps, cuts, surgery, broken bones, and childbirth are some common sources.
The intensity of acute pain varies a lot, and so can the duration. It can pass in an instant or last up to a few months while an injury heals. But once the underlying cause is gone, acute pain goes away, and our lives return to normal.
Chronic pain is a diffuse, aching sensation that lasts much longer than acute pain. In many cases, the cause is unknown. In others, it starts as acute pain, but then it doesn’t go away like it should. Instead, pain signals continue even after the damaged tissue heals.
Chronic pain has no benefit. In fact, it usually has a negative impact on a person’s day-to-day life. Headaches (especially migraines), nerve pain, cancer pain, and fibromyalgia are some examples.
Emotional Pain ranges from social discomfort and stress to grief, anxiety, and depression. We all experience some form of emotional pain at one time or another.
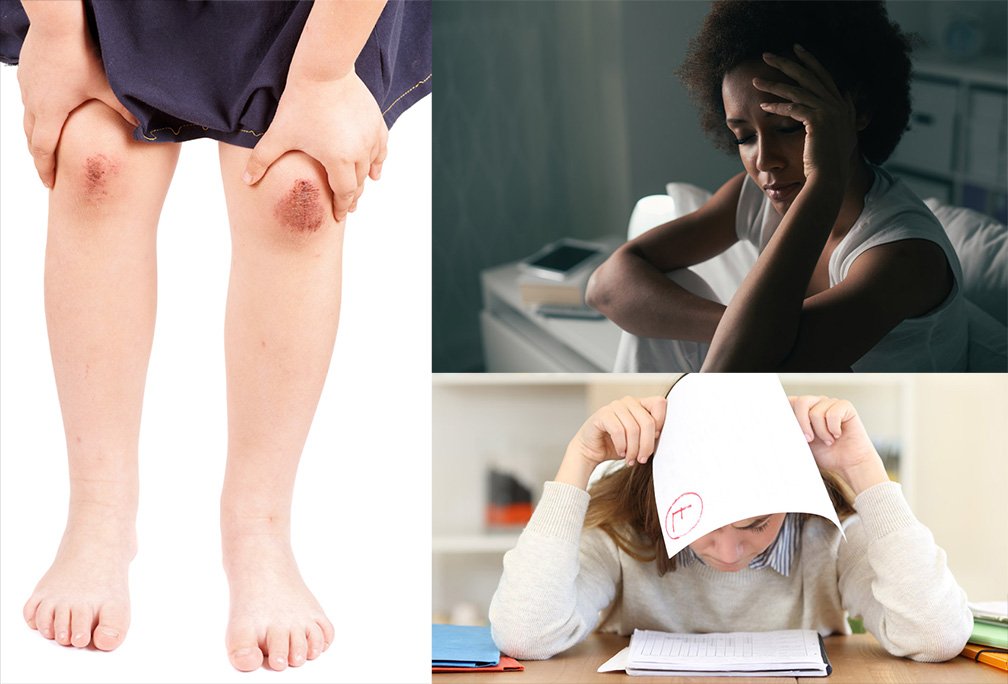
Acute pain (left) comes from an immediate cause, like a skinned knee. Chronic pain (upper right) affects and 25% of people, interfering with their daily life. Stress (lower right) is a common cause of emotional pain.