What is Alzheimer's disease?
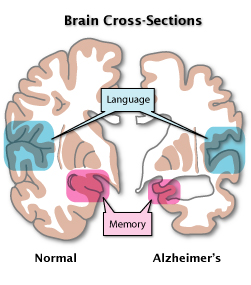
Alzheimer's is a disease that causes dementia, or loss of brain function. It affects the parts of the brain that are important for memory, thought, and language.
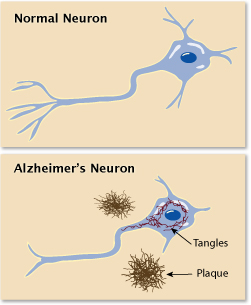
The brain of a person with Alzheimer's contains abnormal clumps of cellular debris and protein (plaques) and collapsed microtubules (support structures inside the cell). Microtubule collapse is caused by a malfunctioning protein called tau, which normally stabalizes the microtubules. In Alzheimer's patients, tau proteins instead cluster together to form disabling plaques and tangles. These plaques and tangles damage the healthy cells around them, leading to cell death. The brain also produces smaller amounts of neurotransmitters (acetylcholine, serotonin, and norepinephrine), chemicals that allow nerve cells to talk to one another.
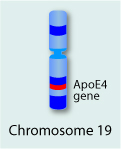
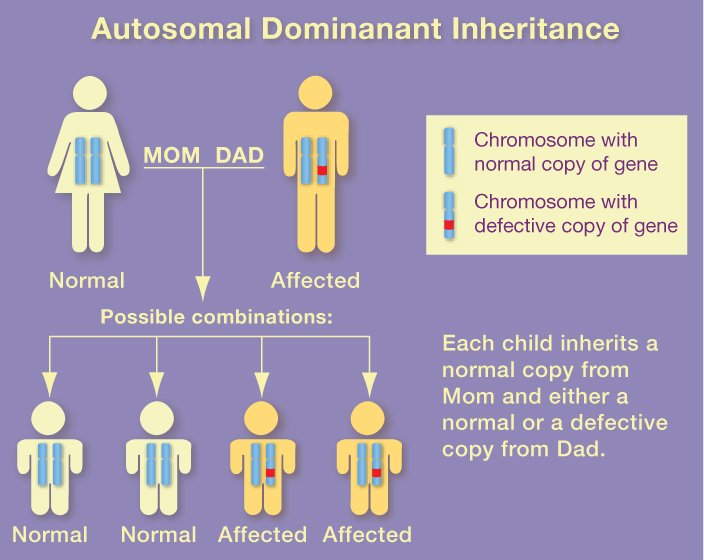
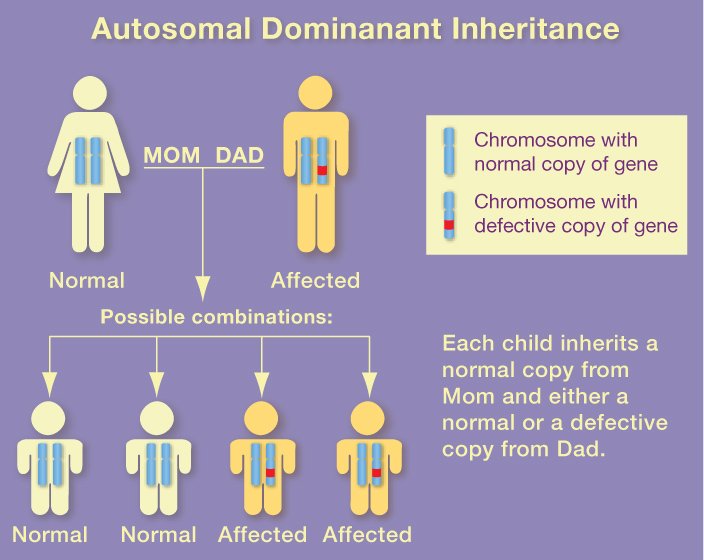
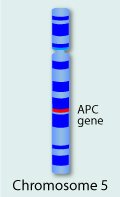
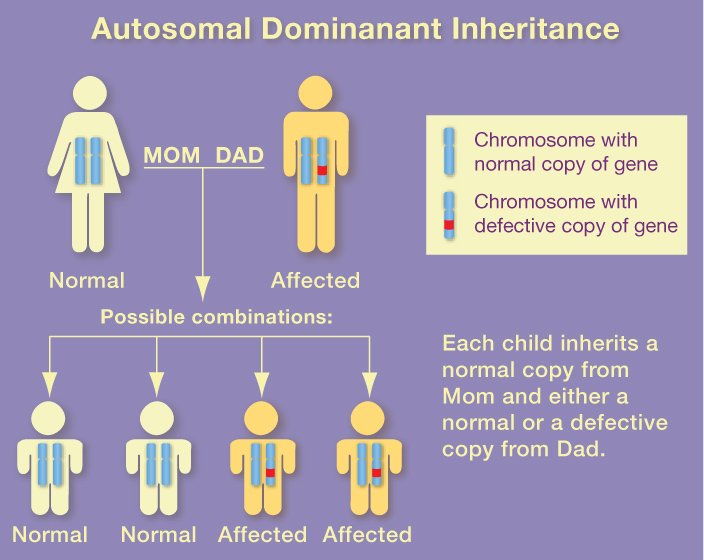
The most common form of the disease, which strikes after age 65, is linked to the apolipoprotein E (apoE) gene on chromosome 19. Scientists don't know how apoE4 increases the risk of developing Alzheimer's. They do know that everyone has apoE, which comes in three forms.
One of the forms (apoE4) increases a person's risk of developing Alzheimer's. The other two forms seem to protect against the disease. While people who inherit the apoE4 form of the gene are at increased risk for the disease, they will not necessarily develop it.
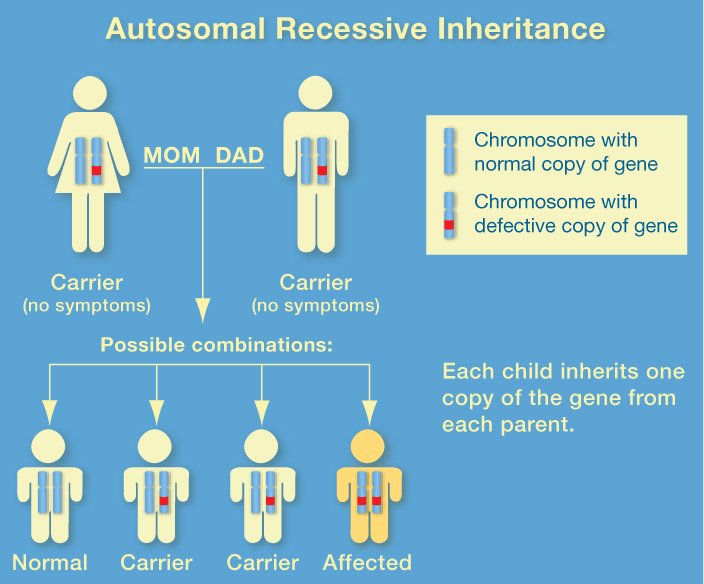
Mutations in genes found on chromosomes 1, 14, and 21 are linked to rarer forms of the disease, which strike earlier in life.
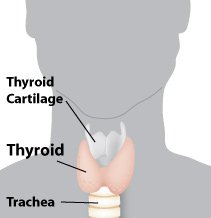
 The thyroid is the largest endocrine gland in the body. It sits just below the larynx (voice box)
and wraps around the trachea (windpipe). The thyroid gland produces thyroid hormone, which helps
the body grow and develop. It also plays an important role in the body's metabolism
(the processes in the body that use energy, such as eating, breathing, and regulating heat).
The thyroid is the largest endocrine gland in the body. It sits just below the larynx (voice box)
and wraps around the trachea (windpipe). The thyroid gland produces thyroid hormone, which helps
the body grow and develop. It also plays an important role in the body's metabolism
(the processes in the body that use energy, such as eating, breathing, and regulating heat).